Motor neurone disease (MND), also known as amyotrophic lateral sclerosis, is a condition in which patients lose motor independence. This is followed by systematic muscle wastage, which may leave affected people immobile for life. The mechanism and progression of MND has been studied in detail over the last few decades. This body of research has offered a great deal of insight into how cellular energetics, growth and activity contribute to the loss of motor function. In addition, certain specific genes (e.g. SOD1) may play a role in some cases of MND. However, these findings have not yet led to a way to entirely reverse MND. The newest study into this condition, however, has reported new findings on how the size of motion-related nerve cells in the spine is affected in MND. This new information may lead to improved therapies for those affected by MND.
MND is a condition currently thought to affect about 1.9 in every 100,000 people worldwide. However, the United Nations projects that the number of MND patients will increase by 69% over the next quarter-century. This is thought to be related to the aging population, particularly as MND typically affects adults between the ages of 40 to 70. The increased prevalence of MND is estimated to affect numerous regions around the globe, including both developed and developing nations. 10% to 20% of all MND cases are thought to be the result of inherited genetic traits, in which a mutated copy of the gene SOD1 is passed from parent to child. The remainder has no defined etiology (at the time of writing) and are regarded as ‘spontaneously’ or sporadically-acquired MND. The condition as a whole has a number of high-profile patients, including the actor David Niven and the exceptional physicist Stephen Hawking.
MND has been found to be associated with characteristic changes in the mitochondrial function, metabolism and overall growth of the nerve cells at the centre of motor function loss in the disease. They are the motor neurones of the spine, in which SOD1 mutations lead to mis-shapen, dysfunctional units of the enzyme superoxide dismutase 1 (SOD1) can ‘decouple’ the normal processes of energy exchange and use in the mitochondria of these cells. On the other hand, mitochondrial dysfunction also occurs in patients with normal SOD1, which is harder to explain. This ultimately leads to impaired oxidative phosphorylation in the mitochondria of MND patients, which in turn leads to reduced ATP availability in the cell as a whole. ATP acts as the ‘energy currency’ of the body; therefore, cells deprived of the molecule are at an increased risk of death.
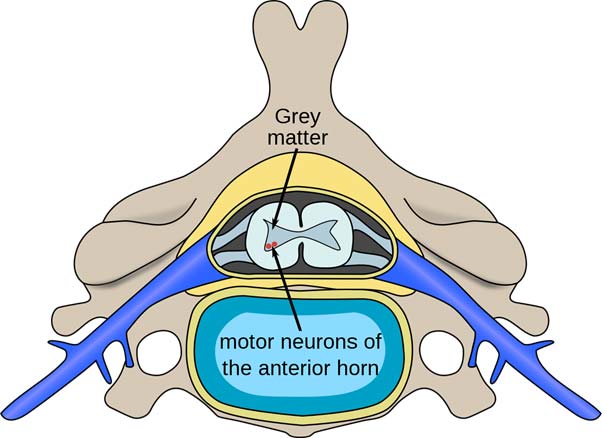
The poliovirus affects the motor neurons of the anterior horn cells, or the ventral (front) grey matter section in the spinal column, which control movement of the trunk and limb muscles including the intercostal muscles. (Public Domain)
These effects, in addition to others such as paradoxical hyermetabolism in the brain and immune system responses, contribute to progressive motor neurone death in animal models of MND. These mice (known as SOD1-G93A mice) exhibit a loss of 70 to 80 percent of their motor neurones. This is associated with the failure of neuro-muscular junctions and the concomitant loss of hind-limb use. This is intended to mirror the progression of MND in human patients. A new study that also used SOD1-G93A mice has resulted in findings that indicate the discovery of a new additional factor in MND initiation and progression: motor neurone size.
This study was conducted at Wright State University, Dayton, Ohio and led by Sherif Elbasiouny at Wright State’s Boonshoft School of Medicine. He and his team focused on the alpha-motor neurones of the spine and their cell bodies, or soma. This region of an individual alpha-motor neurone may indirectly affect its function, which is essentially to interconnect with its surrounding muscle fibres and initiate their contraction, which is the basis of independent movement. Motor neurones require a property called excitability to do this, which is determined by the function and health of its cell body. In addition, the cell body’s function is also related to the energetics and metabolism of the whole cell.
Therefore, motor neurones may fail if the cell body somehow acquires damage or anomaly. In addition, the cell body may need to undergo specific changes during its life-cycle, so as to provide optimal support to the rest of the motor neurone and its functions. Therefore, Elbasiouny and his team conducted two- and three-dimensional studies of alpha-motor neurones in SOD1-G93A mice at various stages of their life-spans and disease progression. They found that these cell bodies were significantly enlarged in SOD1-G93A mice compared to wild-type controls by the tenth and thirtieth days post-birth for each group. These changes relative to normal mice arose prior to MND symptom onset. However, these changes appeared to have been reversed in the ‘test’ mice sixty days later compared to matched controls. This was observed in the remaining populations of motor neurones in the SOD1-G93A mice, as up to 80% of them had died at this point.
Therefore, the cell bodies of alpha-motor neurones (particularly the larger ones) appeared to experience significantly abnormal growth during early-onset MND. The team observed this phenomenon at various points along the spine (i.e. in the cervical, lumbar and sacral spine) in SOD1-G93A mice. This suggests that cell body size is a factor in MND progression, and that this effect is most pronounced and prevalent in larger motor neurones.
On the other hand, this discovery has only been made in one study using an animal model of MND. Furthermore, that model is based on an aggressive, genetic form of the condition, which may represent a reduced proportion of real-life MND cases. Therefore, studies looking for the same cell-body abnormalities in more animal models and in humans are necessary to verify the presence of this new anomaly in all MND cases. Findings such as these may offer greater insights for researchers investigating new and upcoming treatments for the condition.
Top image: Nerve Cells. (Public Domain)
References
Dukkipati SS, Garrett TL, Elbasiouny SM. The vulnerability of spinal motoneurons and soma size plasticity in a mouse model of amyotrophic lateral sclerosis. The Journal of physiology. 2018.
Iyer AK, Jones KJ, Sanders VM, Walker CL. Temporospatial Analysis and New Players in the Immunology of Amyotrophic Lateral Sclerosis. International journal of molecular sciences. 2018;19(2).
Szelechowski M, Amoedo N, Obre E, Leger C, Allard L, Bonneu M, et al. Metabolic Reprogramming in Amyotrophic Lateral Sclerosis. Sci Rep. 2018;8(1):3953.
Arthur KC, Calvo A, Price TR, Geiger JT, Chiò A, Traynor BJ. Projected increase in amyotrophic lateral sclerosis from 2015 to 2040. Nature Communications. 2016;7:12408.
ALSA. What is ALS? ALS Association. 2018. Available at: http://www.alsa.org/about-als/what-is-als.html






No comment