Conditions such as schizophrenia and autism can be difficult to treat and manage, over a lifetime. This may be because scientists' understanding of these conditions has been incomplete, i.e., the treatment could have been unsatisfactory or less than effective for certain patients. On the other hand, researchers working in this area have made progress in leaps and bounds in the last few years.
This advancement, in particular, has led to the identification of hundreds of genetic loci found to be associated with the risk of mental health states. Then again, these loci do not necessarily indicate particular genes; therefore, the development and experience of schizophrenia (for example) are unlikely to be related to something as simple as variations in specific genes. In addition, some studies have concluded that the actual effect of many of these loci on the risk of the condition from patient to patient is variable at best.
Thus, a consortium of researchers from institutions such as the Geffen School of Medicine at UCLA's, SUNY Downstate Medical Center College of Medicine, and the School of Medicine at the University of North Carolina set out to generate a refined model of how these loci affect the more global genome in patients with schizophrenia.
PsychENCODE: The Multi-Dimensional AI Mental Health Genetic Model
This team, known as PsychENCODE, used AI and deep learning to analyze genetic data from relevant studies of the past, including their own, to construct and run this model. This data did not merely concern actual genes and their expression, but all the other applicable genes and loci that influence this expression in turn. These tracts of DNA are known as regulatory networks and include ‘enhancer’ genes and loci that promote the expression of certain other genes more directly involved in brain activity and structure.
These interactions were also modeled in a 3D way: in other words, the possibility that certain genes may be able to affect others, due to the proximity afforded by the way DNA is packed into chromosomes, was also assessed in this model.
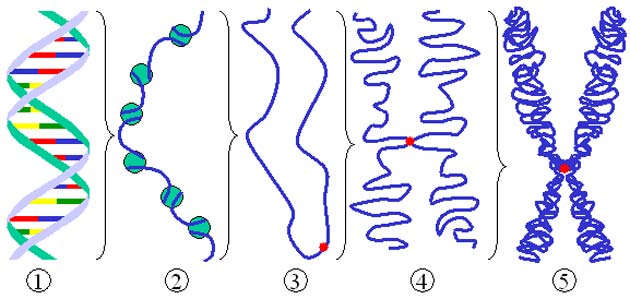
Genes that are far removed from each other in a linear strand of DNA can still potentially interact due to their proximity in the complex, twisted structure of a chromosome. (Source: Public Domain)
The resulting PsychENCODE model was applied to the 142 risk loci for schizophrenia. It revealed that these loci, in fact, regulate 321 additional genes, some of which were identified as factors in the risk of the same condition in previous studies. Therefore, it appears that the new model is powerful enough to track the actual roles of ‘risky’ DNA in this disorder.
The PsychENCODE team also now conclude that their new model can be used to generate similar genetic profiles for other, related mental health conditions. Autism spectrum disorders and bipolar disorders (which are known to have a genetic ‘overlap’ with schizophrenia) are likely candidates for modeling using PsychENCODE, according to the team.
New Model vs. The Old
The group also compared their new model’s output with that of another, more established, one based on the non-regulatory genome alone. They reported that PsychENCODE was the more accurate option.
The researchers behind it now also assert that it can be used to generate more powerful, precise assessments for those who may be at risk of various psychiatric conditions. In addition, it may lead to improved treatments for the patients in question. Therapies (especially those of a medical nature) are recommended based on the genetic-risk profile of the individual with ever-greater frequency. Therefore, the PsychENCODE model, as well as its subsequent generations, may be an effective tool in this form of treatment.
PsychENCODE and the Future
The research and method used to construct this new model can be found in the paper published on the subject in the journal, Science. It is based on the data gathered from the hundreds of studies already done on the genes (and gene-adjacent DNA) that may play a role in conditions such as schizophrenia.
The PsychENCODE project, which was funded by the National Institute of Mental Health (NIMH), may also have helped confirm the authors’ working theory that neurological disorders and the probability of developing one are too complex to define or explain through simple gene-expression activity. Ironically, however, this new AI-powered model may help in putting the rest of their etiology and pathophysiology together, in an easier manner, in the future.
Top Image: Schizophrenia is a mental health condition that may result in feelings of intense paranoia. (Source: Wikimedia Commons)







No comment